The Truth about Living with Neuropathy: Is Life Expectancy Reduced?

Table of Contents
How Long Can You Live With Neuropathy
For many, the persistent tingling in their fingers or numbness in their feet isn’t just an occasional discomfort—it’s the daily reality of living with peripheral neuropathy (PN). While the National Institute of Neurological Disorders and Stroke (NINDS) emphasizes that PN symptoms aren’t directly life-threatening, they often hint at deeper health concerns.
A 2021 study offers a telling perspective: Over 13 years, among 7,116 adults, those with both PN and diabetes had notably higher mortality rates. Specifically, individuals with PN had an average life expectancy of 10.8 years, compared to 13.9 years for those without. This data underscores that while PN may not directly cause death, it’s a significant factor in one’s overall lifespan.
it is important to note that the impact of peripheral neuropathy on life expectancy will vary depending on the individual’s age, overall health, and the severity of their condition
Key Insights:
- Peripheral neuropathy, though not usually fatal, can lead to serious complications if neglected.
- Proper management can ensure a normal life expectancy for those with neuropathy.
- Addressing the root causes and managing symptoms through lifestyle changes are pivotal for overall well-being.

What is Peripheral Neuropathy?
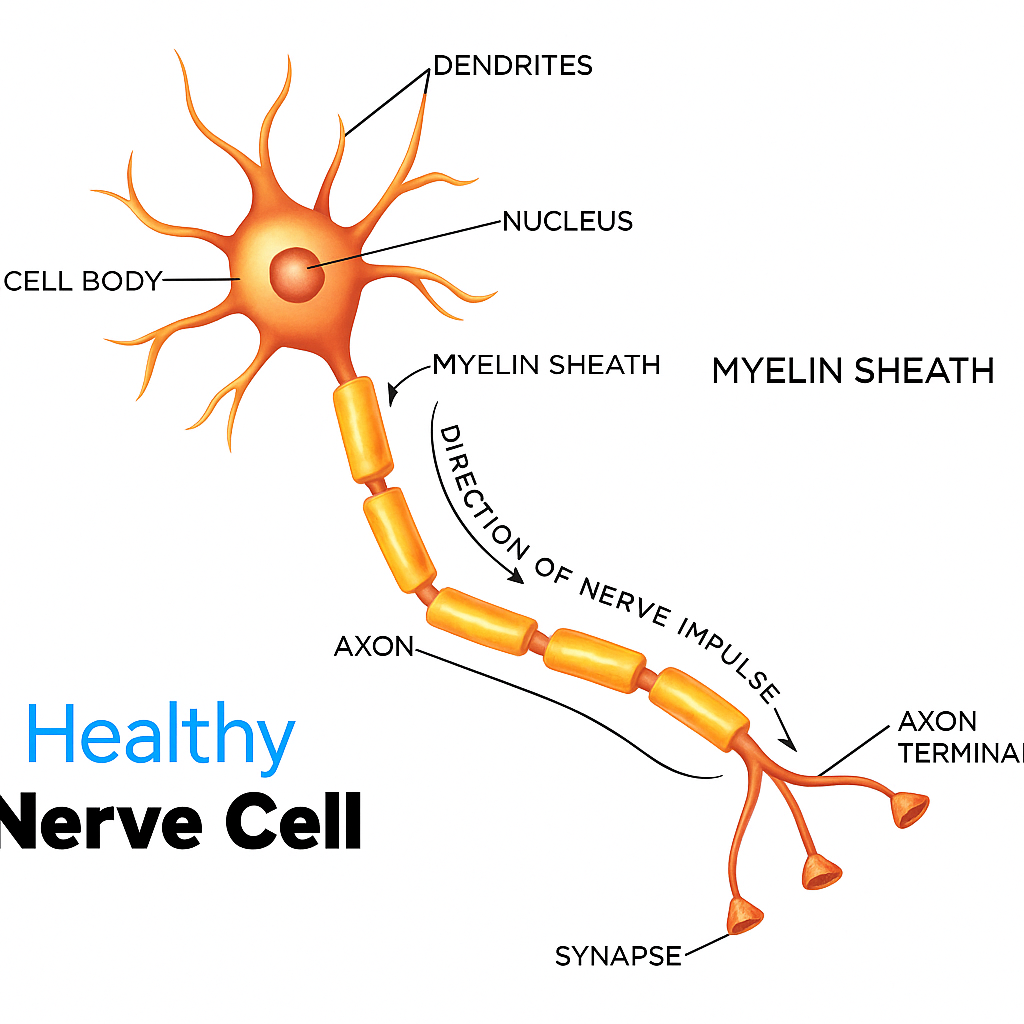
Peripheral neuropathy is a disorder that arises from damage to the peripheral nerves, which serve as the communication bridge between your central nervous system and the rest of your body. This condition can manifest in a range of symptoms such as numbness or tingling in your extremities to muscle weakness or even intense burning pain. A myriad of diseases and factors, with diabetes being a notable one, can trigger this nerve issue.
The emergence of these symptoms necessitates immediate medical attention. Early intervention is not just about managing the discomfort but also about preserving overall health.
The Impact on Life Expectancy
If left untreated, severe peripheral neuropathy can directly reduce life expectancy. The nerve damage can worsen over time leading to loss of sensation, muscle atrophy, and declining mobility. This can profoundly impact one’s ability to perform daily tasks and live independently. Proper medical treatment is key to managing neuropathy and maintaining a normal lifespan.
“While peripheral neuropathy itself may not directly reduce life expectancy, it is imperative that patients take steps to manage it properly. Unchecked, it can lead to significant complications affecting overall health.” – Dr. Taylor Moore
Risk of Serious Complications
Beyond reduced life expectancy, untreated peripheral neuropathy can also lead to serious medical complications. These include skin ulcers or infections due to loss of sensation and impaired wound healing. In some cases, amputation may even be required if damage is left unchecked.
Additionally, injuries or falls become more likely as coordination and balance are affected. Working closely with healthcare professionals can help prevent further deterioration and disability.
Living a Fulfilling Life with Neuropathy
Though peripheral neuropathy presents daily challenges, it does not preclude living a fulfilling life with proper management. By developing an effective treatment plan, making lifestyle adjustments, and taking a proactive self-care approach, many patients control their symptoms successfully.
“Peripheral neuropathy can be a challenging condition, but with proper management many patients find they can maintain a high quality of life,” notes Dr. Zach Bruley, a specialist in peripheral neuropathy treatment.
While symptoms may fluctuate, patients can modify activities and utilize resources like mobility aids and support groups. With education and determination to manage neuropathy proactively, patients can thrive. Though diagnosis may seem overwhelming initially, the prognosis is compatible with enjoying life fully.
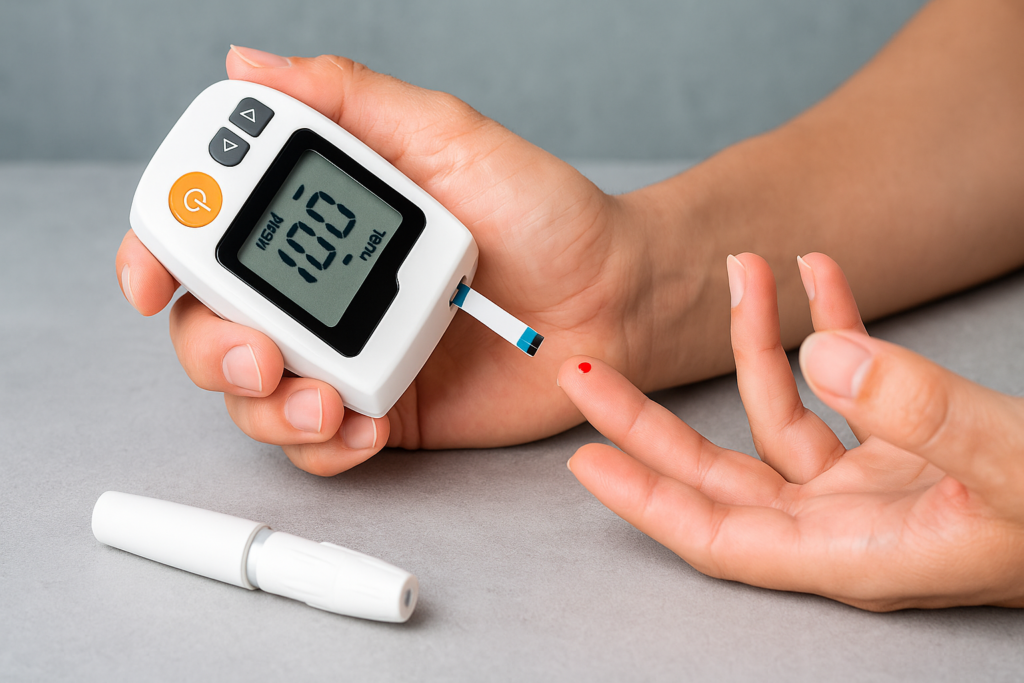
Factors That Can Worsen Neuropathy
Certain factors can exacerbate your neuropathy symptoms, making your condition more severe. It’s crucial to be aware of these potential triggers:
-
Poor Blood Sugar Control: For those with diabetes, maintaining optimal blood sugar levels is essential for managing neuropathy. Poorly controlled blood sugar can lead to nerve damage and exacerbate symptoms.
-
Excessive Alcohol Consumption: Drinking excessively can lead to nutritional deficiencies, which can negatively impact the nerves and intensify neuropathy symptoms.
-
Medications: Some medications, such as specific chemotherapy drugs or those used to treat infections or autoimmune diseases, can cause peripheral neuropathy as a side effect or worsen existing symptoms.
-
Nutritional Deficiencies: A lack of essential vitamins and minerals, especially vitamins B12 and E, folate, and iron, can contribute to nerve damage and amplify the severity of neuropathy symptoms.
The Final Stages of Neuropathy
In the advanced stages of neuropathy, individuals may experience persistent and severe symptoms. The nerve damage can become extensive, leading to a significant reduction in sensation and mobility. Patients might also develop complications like skin ulcers or infections due to impaired wound healing. These advanced stages can profoundly impact daily life and necessitate specialized care and management strategies. It’s important for patients to collaborate closely with healthcare professionals to address symptoms, prevent further deterioration, and enhance their overall quality of life.
Managing Symptoms and Pain
Effectively treating neuropathy symptoms and managing pain is vital for improving your quality of life. Here are some strategies and options to consider:
-
Physical Therapy: Engaging in specific exercises and physical activities can help enhance your balance, strength, and coordination. This can improve your ability to perform daily tasks and reduce the risk of falls or injuries.
-
Medications: Drugs like gabapentin or pregabalin may be prescribed to alleviate nerve pain associated with peripheral neuropathy. These medications work by reducing abnormal nerve firing, which can help relieve discomfort.
-
Topical Treatments: Creams or gels containing capsaicin (an active ingredient found in chili peppers) may offer temporary relief from neuropathic pain. These treatments block certain nerve receptors responsible for transmitting pain signals.
-
Transcutaneous Electrical Nerve Stimulation (TENS): TENS involves using a small device that delivers low-level electrical currents through electrodes placed on the skin. This can help reduce pain by stimulating nerves and promoting the release of endorphins, the body’s natural pain relievers.
-
Chiropractic Care: Spinal manipulation and mobilization techniques performed by chiropractors can help relieve nerve compression and reduce associated pain and inflammation.
-
Compression Socks: Wearing compression socks can aid in managing neuropathy pain, especially in the legs and feet. These socks promote better blood circulation, reduce swelling, and provide support to the affected areas. By enhancing blood flow, they can help alleviate discomfort and pain associated with neuropathy. Finding the best compression socks helps relieve pain!
-
Lifestyle Modifications: Making specific lifestyle changes can significantly impact managing neuropathy symptoms. This includes maintaining a healthy diet, exercising regularly, avoiding excessive alcohol consumption, quitting smoking, and managing underlying conditions like diabetes effectively.
-
Surgery: In severe cases that do not respond to other treatments, surgery may be an option to relieve nerve compression. Procedures like nerve decompression can help mitigate pain and neurological deficits.
“There are many effective options available today to help alleviate neuropathic pain, including medications, physical therapy, and lifestyle changes. Finding the right treatment plan is key.” – Dr. Evan Norum
Address Underlying Causes
Addressing the root causes of peripheral neuropathy is essential for effective treatment. Here are some key considerations:
-
Correcting Underlying Causes: Addressing the root cause can lead to the resolution of neuropathy as nerves recover or regenerate.
-
Identifying the Cause: Neuropathy can result from various factors, including traumatic injuries, infections, metabolic issues, inherited causes, and exposure to toxins. Recognizing and treating the specific cause is crucial for a comprehensive treatment plan.
-
Managing Associated Conditions: If neuropathy results from diabetes, for instance, proper blood sugar control and managing related conditions can help alleviate symptoms.
Can Neuropathy Be Reversed?
While peripheral neuropathy was previously thought to be largely irreversible, new research indicates that certain types may be reversed with proper treatment and management.
The potential for reversibility depends on several key factors:
-
Cause of neuropathy – Neuropathies resulting from removable causes like medication side effects, vitamin deficiencies, or alcoholism tend to have the highest chances of reversal once the underlying trigger is addressed.
-
Timely diagnosis and treatment – Early intervention while neurological damage is still minimal increases the likelihood of full or partial reversal.
-
Individual circumstances – Age, lifestyle factors, and the presence of other medical conditions impact reversibility prospects.
-
Type of neuropathy – Some forms like diabetic neuropathy can be managed but are less likely to be fully reversed. Others like Guillain-Barré syndrome often naturally reverse over time.
According to research, peripheral neuropathies that may be reversible include:
-
Bortezomib-induced neuropathy – Often improves after stopping the chemotherapy drug.
-
Idiopathic neuropathy – Partial reversal is possible with immune-modulating therapies.
-
Nutritional deficiencies – Correcting vitamin B12, folate or iron deficits can allow nerve regeneration.
-
Alcoholic neuropathy – Abstaining from alcohol can enable nerves to heal over time.
-
Autoimmune neuropathies – Treatment of the autoimmune condition may resolve associated neuropathy.
While reversibility is not guaranteed and varies for each patient, prompt evaluation and tailored management offer the best chance of restoring nerve function. Patients should consult a neurologist to determine the prognosis and optimal treatment plan. With a proactive approach, it may be possible to reverse even long-standing neuropathy.

More Information on Lifestyle Modifications
Making specific lifestyle changes can significantly enhance your quality of life while living with neuropathy. Here are some self-care tips to help you manage your symptoms effectively:
-
Exercise Regularly: Engaging in regular physical activity, such as walking or swimming, can improve muscle strength, increase blood flow to nerve endings, and prevent muscle atrophy.
-
Maintain a Healthy Diet: Consuming a balanced diet with plenty of fruits, vegetables, whole grains, and lean proteins can provide essential nutrients for nerve health. Knowing which foods to avoid to goes a long way in helping neuropathy pain symptoms.
-
Manage Stress Levels: Stress can exacerbate neuropathy symptoms, so finding healthy ways to cope is essential. Consider relaxation techniques like deep breathing exercises or meditation.
-
Quit Smoking: Smoking restricts blood flow and impairs circulation, which can further damage nerves affected by neuropathy. Quitting is a vital step towards improving overall health.
-
Practice Good Sleep Habits: Ensuring adequate, restful sleep is essential for managing neuropathy symptoms. Establish a regular sleep routine and create a conducive sleeping environment.
-
Protect Extremities: Since peripheral neuropathy often affects the extremities, taking extra precautions to avoid injuries or infections is essential. Regularly inspect your feet for any cuts or sores, wear protective gloves when necessary, and choose appropriate footwear.
Adaptive Strategies for Daily Activities
Living with neuropathy can present challenges in daily tasks. However, adaptive strategies can make these activities more manageable:
-
Use Assistive Devices: Tools like grip aids, reachers, and button hooks can assist with tasks like opening jars or fastening buttons.
-
Modify Living Spaces: Adjust your home to accommodate your needs. Install handrails in bathrooms, and consider using ramps instead of stairs if mobility is an issue.
-
Manage Pain: Take breaks as needed to avoid overexertion and prevent pain flare-ups. Use relaxation techniques to alleviate discomfort.
-
Prioritize Safety: Ensure pathways are clear of clutter or hazards that could increase the risk of falls. Install adequate lighting and use non-slip mats in potentially slippery areas.
-
Plan Ahead: Break tasks into smaller steps to make them more manageable. Create schedules or reminders to help you stay organized.
-
Seek Support: Connect with support groups or online communities to share experiences, tips, and resources.
Neuropathy FAQs: Unraveling the Facts
What Causes Peripheral Neuropathy?
The origins of peripheral neuropathy are diverse, including medical conditions like diabetes, autoimmune diseases, infections, toxin exposure, and certain medications like chemotherapy agents. Genetics, physical injuries, and lifestyle choices can also play a role.
What are the Symptoms of Peripheral Neuropathy?
Symptoms can vary, with common indicators including numbness, tingling, burning sensations, muscle weakness, and coordination challenges. While hands and feet are frequently affected, symptoms can manifest in other body parts as well.
Is There a Cure for Neuropathy?
Currently, there isn’t a universal cure for neuropathy. However, a plethora of treatments and management techniques exist that can alleviate symptoms and slow its progression.
How Can Lifestyle Changes Impact Neuropathy?
Embracing specific lifestyle shifts can make a significant difference. A nutritious diet, regular physical activity, effective stress management, and avoiding harmful substances like alcohol or tobacco can play pivotal roles in managing and mitigating neuropathy symptoms.
Conclusion
Neuropathy, while undeniably challenging, doesn’t have to define one’s quality of life. With the right resources, proactive care, and a touch of resilience, individuals can indeed lead fulfilling lives. For anyone facing the intricacies of neuropathy, remember: knowledge is power. Seek expert medical guidance, harness the vast array of available resources, and embark on this journey with confidence and hope.

OFFICE HOURS
Monday
10:00am – 1:00pm
3:00pm – 6:00pm
Tuesday
3:00pm – 6:00pm
Wednesday
8:00am – 12:00pm
3:00pm – 6:00pm
Thursday
10:00am – 1:00pm
3:00pm – 6:00pm
Friday
Closed
Saturday
Closed

About the Author
Dr. Evan Norum, co-owner of Advantage Chiropractic in New Berlin, WI, holds a Doctorate of Chiropractic from Northwestern Health Sciences University. Inspired by personal experiences with chiropractic care, he specializes in family-based treatments and is board-certified in chiropractic care, neuropathy, and the Torque Release Technique®. With internships at leading chiropractic centers and co-founding Advantage Chiropractic in 2017, Dr. Evan Norum is dedicated to promoting health from within.

